Health Promotion
Policy change is a powerful way to make environments – where people live, work, play, learn, and shop – become more supportive of adopting healthy behaviors for everyone.
Modifiable risk factors cause a large proportion of cancer cases and deaths. A recent study shows that an estimated 40% of all cancer cases and 44% of cancer deaths in the United States are attributable to a combination of modifiable risk factors, including tobacco use, excess body fatness, and alcohol consumption.
Reducing the prevalence of these risk factors can help mitigate the cancer burden, but individual-focused initiatives are unlikely to succeed without addressing the external factors that influence behaviors. To be effective, health promotion efforts must tackle the environmental, economic, and social factors that influence an individual’s opportunities to engage in healthier behaviors. This is especially important in the context of health equity, as underserved communities are most exposed to environments that are not conducive to adopting healthy behaviors (see Cancer in Indigenous Populations). Policy change is a means to ensure environments are increasingly supportive of the adoption of healthy behaviors by everyone (see Policies and Legislation).
To encourage policy change and promote healthy diets and physical activity, the World Cancer Research Fund International (WCRF) has created the NOURISHING and MOVING policy frameworks (Figure 33.1). The NOURISHING framework consists of 10 key policy areas within three domains: food environment, food system, and behavior change communication. The MOVING framework consists of six policy areas across four domains: active societies, active environments, active people, and active systems.
World Cancer Research Fund International (WCRF) NOURISHING and MOVING Frameworks
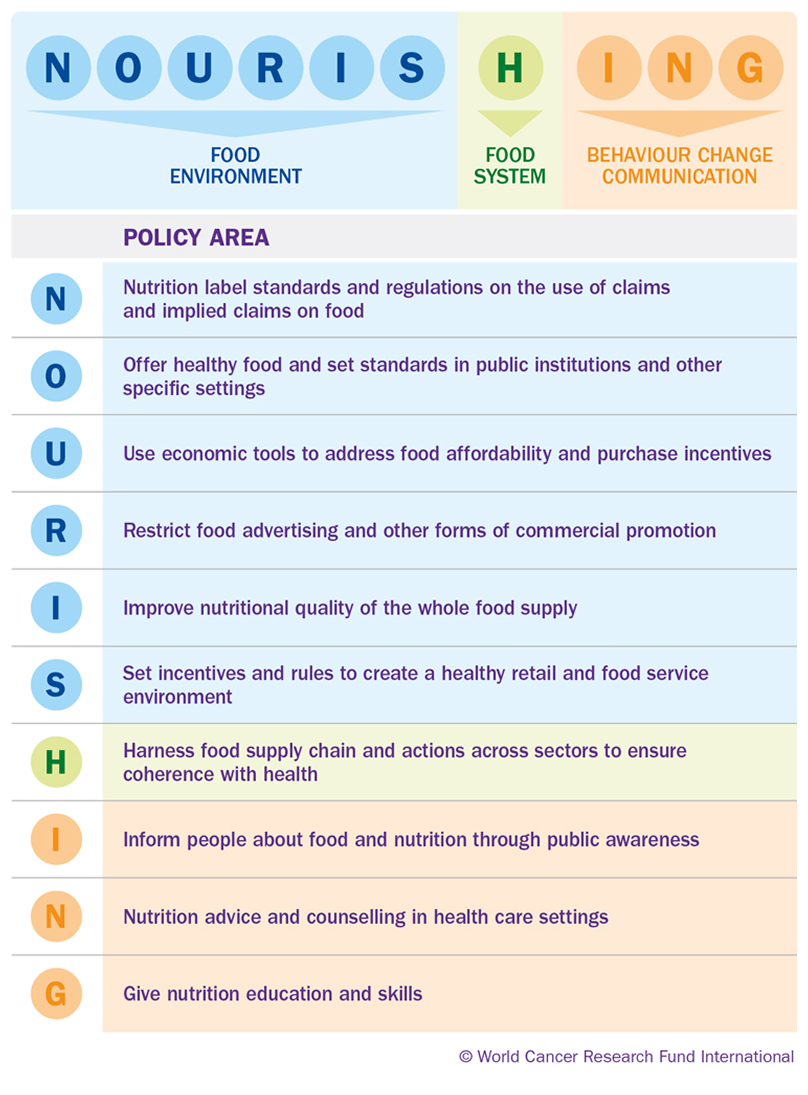

“The choices we make are shaped by the choices we have. Let’s create better choices for everyone.”
Although the comprehensive set of nutrition and physical policies outlined in these frameworks have yet to be fully achieved, there are notable examples of progress. These include offering healthy foods in public institutions in the European Union (Figure 33.2) and city and regional efforts to implement a more sustainable, local food system (Figure 33.3).
Children participating in School Scheme providing fresh fruit, vegetables, and milk, by country in Europe, 2022-2023
Local Food Policy for a more sustainable, local food system – example from Ghent, Belgium

“When people can’t make the healthy choice because their environment is stacked against them, we’re failing as a society.”
The Food Is Medicine Initiative is a tailored food-based nutritional intervention linked to the health care system intended to control chronic diseases, and often addresses food and nutrition insecurity and has recently gained traction in the US. As of January 1, 2024, 11 states have applied for special legal permissions to provide nutrition interventions for Medicaid enrollees (Map 33.1).
Moreover, there is increased recognition that policies aimed at reducing alcohol consumption and raising awareness about its health hazards are essential for lowering cancer risk (see Alcohol) (Figure 33.4).
Alcohol warning labels in Ireland

